Commercial Insurance Billing Terms: Essential Guide
Commercial insurance billing is where “good enough” processes get exposed fast: plan-specific edits, prior auth traps, COB landmines, silent network changes, and denial logic that never shows up in a policy PDF. If your team is guessing instead of proving eligibility, benefits, and documentation alignment, you’ll bleed cash through avoidable write-offs, rework, and missed timely-filing windows. This guide is built to make your workflows denial-resistant—so you can translate payer language into operational steps, defend every payment, and stop revenue leakage before it hits AR.
1) Commercial Insurance Billing: How It Actually Breaks (And Where Teams Lose Money)
Commercial payers don’t deny because you “coded wrong” in the abstract—they deny because one specific rule wasn’t satisfied, evidenced, or transmitted the way that plan expects. Your team needs a repeatable way to translate payer behavior into controls: eligibility capture, benefits validation, authorization evidence, documentation alignment, claim formatting, and denial playbooks.
Where commercial billing gets expensive (fast):
Eligibility is treated as a yes/no, not a data record. “Active” is meaningless if the plan is active under the wrong member ID, wrong group, wrong product type, or wrong effective date. Capture eligibility as structured data tied to a claim and supported by the remittance logic you’ll see in the Explanation of Benefits (EOB) and downstream CARCs + RARCs.
Benefits are verified verbally but not mapped to billing actions. Coverage isn’t compliance. Your “covered” service can still be nonpayable if medical necessity criteria aren’t met, so benefits verification must reference a written necessity standard and documentation plan (use a medical necessity checklist from your medical necessity criteria guide).
Authorization evidence is weak or scattered. Commercial payers deny with confidence when auth numbers are missing, mismatched, expired, or don’t match CPT/units. Treat auth as an audit artifact with attached workpapers—use the same discipline you’d use in a medical coding audit.
COB is “someone else’s problem.” Coordination errors don’t just delay payment—they create wrong payer billing, refunds, recoupments, and secondary denials. Build COB into intake and resubmission strategy using your coordination of benefits (COB) definitions.
Edits and modifiers get treated like trivia. Commercial edits often mirror NCCI-style thinking, but payer-specific bundling and modifier logic can differ. If your team can’t explain why a modifier is present, you’re inviting denials—tighten with a modifier/edit workflow based on coding edits and modifiers.
Commercial success looks like this: your billing team can read an EOB, translate denial language into root cause, fix the upstream process (not just resubmit), and measure the result using RCM KPIs. If you’re not doing that, you’re paying denial tax—through rework, aging AR, and silent revenue leakage.
2) Eligibility + Benefits Verification That Holds Up Under Denials
“Eligibility verified” is not a checkbox—it’s a mini-audit record that must survive denials, patient disputes, and payer reversals. Your goal is to ensure that when a claim denies, you can answer three questions immediately:
Was the patient eligible on the date of service?
Was the benefit payable for this setting/provider?
Did we meet plan rules (auth/referral/medical necessity/documentation)?
Build an eligibility record, not a conversation
Stop relying on memory or call-center statements. Capture these fields every time:
Member ID, group, product name, effective dates, plan type, network status
Accumulators (deductible met, OOP status), copay/coinsurance by benefit
Auth/referral requirements by CPT category
Coverage limitations (visit caps, frequency, site-of-service constraints)
Then, tie your eligibility record to the claim outcome using your EOB workflow and reason-code translation via CARCs and RARCs. This is how you convert payer “because we said so” into a fixable root cause.
Benefits verification must produce billing actions
Benefits are only useful if they change what you do next. Example: if benefits show deductible applies and coinsurance is high, your front-end collections and patient communication must change—and you should monitor the impact in RCM KPIs (POS collection rate, bad debt %, days in AR).
Medical necessity is where most “coverage” collapses
Commercial plans frequently pay only when clinical documentation aligns with policy criteria. That means your benefit verification must include a documentation plan:
What diagnosis specificity is needed?
What exam elements or objective findings must be documented?
What prior conservative treatment history must be present?
What risk/complexity must be explicit?
Use a structured checklist grounded in medical necessity criteria and supported by strong documentation integrity via CDI terminology. If your coders are constantly “waiting for better notes,” you don’t have a coder problem—you have a revenue protection problem.
Don’t let COB become a denial factory
COB failures create denials that look like payer errors but are really workflow failures. Every visit should confirm insurance order and coverage status—especially if the patient changed jobs, changed plans, added a spouse plan, or moved between plan products. Use COB definitions and rules to build scripts and intake checks that prevent “wrong payer billed” rejections that push you toward timely filing risk.
3) Authorizations, Referrals, and Documentation: Turning “We Think We Have It” Into Proof
Commercial payers don’t reward effort. They reward evidence. Most orgs lose appeals because they can’t produce a clean, chronological packet that proves compliance with plan requirements.
Authorization controls that actually prevent denials
A denial-proof authorization workflow has four layers:
Scope match: authorized CPT family, units, DOS range, site of service, provider
Identity match: member ID/group + rendering/billing NPI alignment
Evidence: screenshot/letter + call reference + notes + timestamps
Claim transmission: auth number placed where payer expects it
Treat the authorization packet like workpapers from an audit—consistent naming, stored evidence, and easy retrieval. If you already train staff on audit language, borrow structure from your medical coding audit terms dictionary and general financial audits guidance.
Documentation integrity is a billing control (not “provider education”)
Commercial payers deny when documentation is vague, templated, or missing the clinical logic that maps to policy. Your documentation standard should:
Force diagnosis specificity and clinical justification
Tie services to necessity (why now, why this intensity, why this setting)
Support modifier usage with explicit facts (distinct procedure, separate site, separate encounter, etc.)
Use CDI terms to standardize prompts, and reduce denials rooted in “insufficient documentation” or “not medically necessary” by aligning with medical necessity criteria.
Edits/modifiers: require justification, not habits
Commercial edits punish “default modifier culture.” If your staff routinely adds modifiers “because it worked last time,” you will eventually trigger systemic denials. Build a rule: every modifier needs a documented justification and should be tested against payer behavior using coding edits and modifiers and validated against the payer’s remittance logic (again: EOB, CARCs, RARCs).
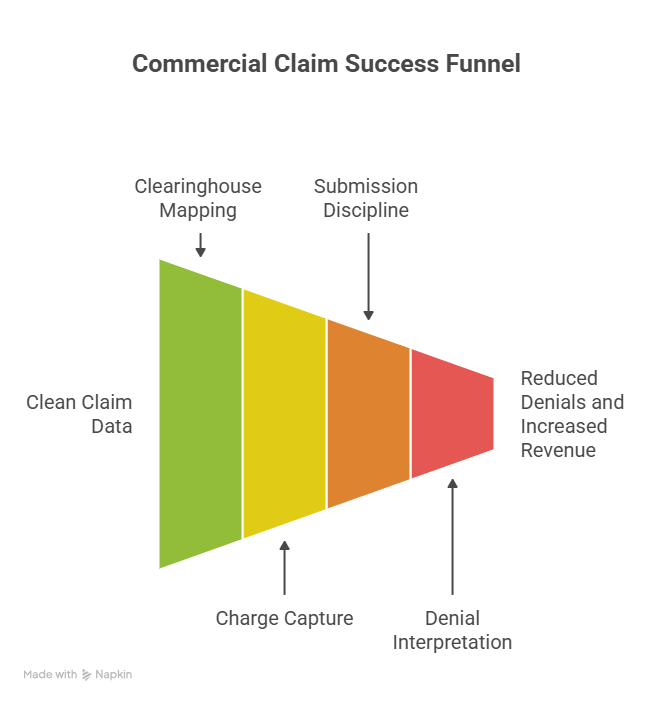
4) Claims That Clear: Data Integrity, Clearinghouses, and Submission Discipline
Commercial claim success is mostly upstream discipline: clean demographics, correct payer routing, accurate provider identifiers, and submission formats that survive payer edits.
Clearinghouse issues create “invisible” systemic loss
When a clearinghouse mapping breaks, you can see spikes in rejections, missing attachments, or payer-specific formatting issues. Your team must understand routing, scrubbing, and payer acceptance behavior using a shared language from the clearinghouse terminology guide. This is a control point—treat it like infrastructure.
Charge capture is where commercial revenue leaks first
Commercial claims can be “perfectly coded” and still underbill if charges were never captured, units were wrong, or ancillary services weren’t tied to documentation. Hardening charge capture prevents denials and prevents missing revenue—use charge capture terms plus a leakage mindset from revenue leakage prevention.
Submission discipline: prevent timely filing disasters
Rejections are not harmless—they burn days, trigger rework, and can push claims past timely filing limits (especially for corrected claims). Use a language framework from medical claims submission terminology and measure performance in RCM KPIs such as clean claim rate, rejection rate by payer, and “days to first submission.”
Denials and edits: your remittance is the curriculum
Train your team to interpret remittance precisely:
What did the payer do? (denied, bundled, downcoded, applied deductible, shifted liability)
Why? (reason code logic)
What evidence would reverse it? (auth proof, documentation, COB proof, corrected claim, appeal packet)
Your playbook should be built on EOB interpretation and reason-code mastery via CARCs + RARCs. When you do this right, denial categories shrink over time because fixes move upstream—not because your follow-up team is “working harder.”
5) Denials, Appeals, and Underpayments: Build a Commercial Payer Defense System
A denial management program is not a queue—it’s a feedback system that stops repeats.
Step 1: Categorize denials by control failure
Instead of “denial reason,” classify by what broke:
Front-end: eligibility, benefits, COB, auth/referral
Clinical evidence: medical necessity, documentation specificity, CDI gaps
Coding/submission: modifiers, bundling edits, claim formatting, missing data
Contract/payment: underpayment, incorrect allowed, misapplied adjustments
Use standardized language (and staff training) based on RCM KPI definitions and audit discipline from financial audits so reporting is consistent and actionable.
Step 2: Build appeal packets that win
Winning appeals isn’t about emotion. It’s about proof:
eligibility proof (portal capture/call log)
authorization/referral proof (letter + number + scope)
medical necessity proof (policy criteria + documented facts)
coding rationale (modifier justification + note support)
remittance logic (EOB + CARC/RARC interpretation)
If your packets are weak, your appeals become busywork. Train packet structure using EOB fundamentals and denial language from CARCs/RARCs.
Step 3: Underpayment detection is a profit center
Commercial underpayments are common because most practices don’t reconcile expected allowed vs paid at the line level. Even without perfect contract tech, you can:
target top CPTs and high-volume payers
compare paid vs historical norms
flag anomalies (sudden drop in allowed, new bundling behavior, missing add-on payments)
Underpayments are often disguised as “contractual adjustments.” If posting is sloppy, you’ll never find them. Tie underpayment audits to revenue leakage prevention and measure results through RCM KPIs.
Step 4: Reduce repeat denials with documentation + process redesign
When “insufficient documentation” repeats, your fix is not “tell providers to document better.” Your fix is:
create a templated medical necessity checklist per service category
build CDI prompts at point of care using shared terms from the CDI dictionary
enforce modifier justification rules from edits/modifiers guide
validate outcomes via remittance analysis (EOB/CARC/RARC)
That’s how denial volume drops while cash accelerates.
6) FAQs: Commercial Insurance Billing Questions That Actually Matter
-
-
If the payer rejected/denied due to incorrect claim data (missing info, wrong ID, wrong provider fields), it’s often a corrected claim path. If the payer adjudicated and you’re disputing the decision based on coverage/necessity/contract logic, it’s an appeal path. Your remittance language (EOB + reason codes) should drive the routing—use EOB guidance and translate via CARCs.
-
Because “active” doesn’t validate product, effective date, network rules, or payer order. The patient can be active under a different plan variant, a changed group/product, or secondary status under COB. Build intake and visit-level verification using COB rules and store evidence that can defend the claim later.
-
Documentation that fails to map to payer criteria: missing objective findings, no prior conservative treatment history, vague diagnoses, or unclear reason for intensity/frequency. Fix it by standardizing checklists using medical necessity criteria and reinforcing with point-of-care prompts using the CDI dictionary.
-
Make COB a mandatory re-verification step at each visit and at any demographic change. Train staff to capture primary/secondary order and plan changes, and document proof. Use a shared rule language from COB definitions and track denial volume reductions via RCM KPIs.
-
Start with focus: top payers + top CPTs. Compare paid allowed amounts to historical norms and flag sudden drops. Use remittance reason codes and posting discipline to separate real contractual adjustments from underpayments, and connect findings to revenue leakage prevention. Even simple variance queues can recover meaningful dollars.
-
At minimum: clean claim rate, rejection rate, denial rate by category (front-end vs clinical vs coding/submission vs payment/contract), appeal win rate, days to first submission, and top denial reasons with linked fixes. Define and standardize measures using the RCM metrics & KPIs glossary so leaders stop arguing over definitions and start fixing processes.