Guide to Healthcare Claims Management Terms
Healthcare claims management breaks down when teams use the same words but mean different things operationally. A registrar says the patient is verified, the biller says the claim is clean, the coder says the documentation supports it, and the payer still rejects it. Revenue gets stuck in the gap between definitions and execution.
This guide fixes that gap. It translates the claims terms that control submission, adjudication, denials, payment posting, and recovery work into practical decisions your billing team can actually use to protect cash flow, reduce rework, and stop preventable revenue leakage before it spreads.
1. Healthcare Claims Management Terms That Actually Control Revenue
Healthcare claims management is not just the act of sending a bill. It is the full operating system that moves a service from registration to reimbursement, with risk checks at every stage. If your team does not understand the language behind that system, errors multiply quietly. A small eligibility miss becomes a front-end rejection. A documentation gap turns into a medical necessity denial. A posting error distorts your reporting and hides an underpayment trend. That is why strong claims teams study revenue cycle management terms, tighten their medical claims submission process, and build habits around accurate medical billing and reimbursement instead of treating claims work like simple data entry.
Start with the most dangerous misunderstanding in the department: a rejection is not the same as a denial. A rejection usually means the claim never made it through a clearinghouse or payer intake process because of formatting, missing data, invalid identifiers, or edit failures. A denial means the payer accepted the claim into adjudication and then refused payment fully or partially. Teams that blur those terms create the wrong workflow, waste analyst time, and misreport performance. That is why the vocabulary inside clearinghouse terminology, denials prevention and management, claim adjustment reason codes, and remittance advice remark codes matters so much.
You also need to separate billing terms from cash terms. A billed amount is not an allowed amount. An allowed amount is not a paid amount. A paid amount is not net collectible revenue. And a contractual adjustment is not the same thing as a write-off caused by internal failure. Teams that do not understand that chain make terrible decisions in A/R follow-up because they chase balances that were never collectible and miss balances that absolutely were. That is where knowledge of commercial insurance billing terms, Medicare reimbursement, the physician fee schedule, patient responsibility and copay terms, and payment posting and management stops confusion from turning into write-offs.
Finally, claims management terms only become valuable when they are tied to control points. Eligibility belongs before service. Authorization belongs before high-risk scheduled care. Charge capture belongs immediately after documentation completion. Claim edits belong before submission. CARCs and RARCs belong in structured denial analysis, not scattered across notes. A/R metrics belong in weekly operational review, not month-end panic. Teams that connect language to action outperform teams that merely memorize acronyms from a healthcare billing acronyms dictionary, a medical coding workflow reference, or a generic mastering revenue cycle management guide without operational discipline.
Healthcare Claims Management Terms Map: What They Mean and What You Must Do (28+ Rows)
| Term | What It Means | Why It Hits Claims | Best Practice Action |
|---|---|---|---|
| Clean Claim | A claim complete enough to pass payer edits without manual correction. | Improves first-pass acceptance and reduces rework cost. | Use pre-bill edits and payer-specific rules before submission. |
| Claim Scrubber | Software logic that checks claims for format, coding, and billing errors. | Catches preventable defects before the payer sees them. | Update edit logic regularly and review top edit failures weekly. |
| Front-End Rejection | A rejection before adjudication due to missing, invalid, or mismatched data. | Stops the claim cold and delays cash before payer review begins. | Separate rejection queues from denial queues and assign rapid correction ownership. |
| Payer Denial | A refusal to pay after the claim enters adjudication. | Signals medical, contractual, policy, or documentation failure. | Classify denials by root cause, not only by payer code. |
| Eligibility Verification | Confirmation that coverage is active and benefits align with the service date. | Prevents bad debt and avoidable eligibility denials. | Re-verify near date of service for high-risk visits and procedures. |
| Prior Authorization | Payer approval required before selected services are performed. | Missing authorization can erase payment even when care was appropriate. | Track authorization status with service-level detail, not general notes. |
| Medical Necessity | Proof that the service was clinically justified under payer rules. | A common reason for full denials and downcoding. | Match diagnosis, documentation, and service intensity before billing. |
| Charge Capture | The process of turning documented services into billable charges. | Missed or delayed charges create invisible revenue leakage. | Audit charge lag and compare schedules, notes, and billed services. |
| Claim Edit | A rule checking claims for payer, coding, or compliance issues. | Determines whether the claim is corrected before or after submission. | Maintain payer-specific edit libraries and retire obsolete edits. |
| Adjudication | Payer review that decides payment, reduction, or denial. | This is where contractual logic and policy enforcement hit revenue. | Read remits carefully and compare expected versus actual payment. |
| Allowed Amount | The maximum reimbursable amount under payer rules or contracts. | Determines what portion is collectible and what becomes adjustment. | Model expected reimbursement by payer and service line. |
| Contractual Adjustment | The non-collectible difference between charge and contracted allowance. | Misposting distorts net revenue and collection metrics. | Post using mapped reason logic tied to payer contracts. |
| Patient Responsibility | The patient’s share, such as deductible, copay, or coinsurance. | Poor estimation and posting create collection confusion and complaints. | Estimate up front and reconcile after final adjudication. |
| Coordination of Benefits (COB) | Rules determining which payer is primary, secondary, or tertiary. | Wrong sequencing triggers rejections, denials, and refund cycles. | Validate coverage order before claim release and at every insurance update. |
| Timely Filing Limit | The deadline for original claims, corrected claims, or appeals. | A valid claim becomes worthless once the filing window closes. | Track deadlines separately for originals, rebills, and appeals. |
| CARC | Claim Adjustment Reason Code explaining a payment reduction or denial. | Essential for classifying denial categories correctly. | Pair each CARC with corrective workflow and owner. |
| RARC | Remark code adding payer explanation to the adjustment outcome. | Provides detail needed for appeal, rebill, or documentation follow-up. | Train staff to read CARC and RARC together, never in isolation. |
| ERA | Electronic remittance advice containing payment and adjustment details. | Drives automated posting and denial routing. | Audit ERA mapping so the right balances hit the right queues. |
| EOB | Payer explanation of what was billed, paid, adjusted, or owed. | Often the fastest way to spot underpayment or patient liability errors. | Use EOB review for exception-based follow-up, not blind posting. |
| Corrected Claim | A resubmitted claim replacing an earlier version after billing error correction. | Needed when the original claim itself was wrong. | Use the correct frequency code and payer-specific corrected claim format. |
| Appeal | A formal challenge to a payer’s denial or underpayment decision. | Recovery depends on evidence, timing, and payer-specific requirements. | Build appeal packets from denial type templates, not from scratch. |
| Reconsideration | A payer review request often used before or instead of full appeal. | Can recover money faster when the issue is straightforward. | Match the request type to payer policy and issue type. |
| Underpayment | Payment below contracted or expected reimbursement. | Quietly drains revenue when teams only chase denials. | Run expected-versus-actual payment variance reports by payer. |
| Recoupment | A payer recovery of previously paid funds. | Can erase current cash if not identified and challenged quickly. | Monitor takeback activity and validate recoupment grounds immediately. |
| Write-Off | Balance removal due to contractual, administrative, or bad debt reasons. | Uncontrolled write-offs hide preventable operational loss. | Separate approved contractual write-offs from internal failure write-offs. |
| A/R Days | Average number of days claims remain unpaid in accounts receivable. | Shows whether cash is moving or stalling. | Track by payer, financial class, and denial category. |
| First-Pass Resolution Rate | Percentage of claims paid without rework after first submission. | One of the clearest signals of upstream process quality. | Use it alongside rejection and denial trends, not alone. |
| Net Collection Rate | How much collectible revenue the organization actually collects. | Reveals whether revenue is being recovered or leaking out. | Measure by payer and service line, then assign corrective action. |
2. Terms That Decide Whether a Claim Leaves Your System Correctly
The cleanest denial is the one that never happens because the claim never left your system with a known defect. That sounds simple, but the work is not simple. It starts with source data integrity. If registration captures the wrong subscriber ID, or the patient’s plan sequencing is not updated, the downstream team spends days fixing something that should have been prevented in two minutes. That is why strong claims management always ties front-end workflows to coordination of benefits, patient responsibility terms, practice management systems, and EHR integration terms instead of pretending those are separate departments with separate problems.
Next comes charge capture, and this is where a lot of revenue dies quietly. A claim cannot be accurate if the charge never becomes a claim at all. Missing infusions, unbilled supplies, wrong units, incomplete modifiers, and lagging encounter closeout all create a false sense of productivity because the biller never even sees the missing revenue. This is why sophisticated teams pair charge capture controls with clinical documentation integrity, strong EMR documentation practices, and disciplined use of coding edits and modifiers. When documentation, coding, and billing are disconnected, claims management becomes a repair shop instead of a revenue engine.
Then comes the claim scrubber and the clearinghouse. These terms sound technical, but operationally they answer one question: did your team catch the defect before the payer did? A scrubber is only useful if its edit library reflects current payer behavior, specialty-specific patterns, and recurring internal mistakes. A clearinghouse is only useful if staff know how to interpret reject reports rapidly and route them to the right owner. Teams that dump everything into a generic “claim error” queue lose time, miss filing limits, and distort root-cause reporting. That is why clearinghouse terminology, revenue cycle management software terms, medical coding workflow terms, and the broader claims submission process should be understood by operations staff, not just IT or vendor managers.
One more term matters here: timely filing. Teams often talk about it as a back-end denial issue, but the damage starts up front. Every day a rejected claim sits untouched, every day an unsigned note delays final coding, and every day a missing authorization sits unresolved burns down the filing window. Timely filing is not just a payer rule. It is a pressure test of the entire claims management system. If your organization constantly fights filing-limit denials, the real issue is rarely one late biller. It is usually broken task ownership, slow exception handling, weak revenue leakage prevention, poor HIPAA-compliant billing workflows, and a lack of operational rigor in medical billing compliance.
3. Terms That Explain How Payers Actually Process and Price Claims
Once the claim is accepted for processing, the most important term is adjudication. This is the payer’s decision engine. It checks coverage, contract terms, fee schedules, policy edits, coding logic, authorization status, and medical necessity. If your team cannot explain what happened during adjudication, you are not really managing claims. You are just reacting to remits. High-performing teams train staff to read adjudication outcomes through the lenses of commercial insurance billing, Medicare reimbursement rules, physician fee schedule logic, and accurate reimbursement methodology.
A critical pair of terms here is billed amount versus allowed amount. Your charged amount reflects your fee structure. The allowed amount reflects what the payer says is payable. The difference is often a contractual adjustment, but not always. Sometimes the reduction is caused by bundling edits, modifier problems, unit mismatches, or a non-covered component buried inside the line item. If your team posts adjustments mechanically without checking expected reimbursement, underpayments disappear into the ledger. That is why claims management must connect payer remits to payment posting controls, revenue cycle metrics and KPIs, revenue cycle efficiency benchmarks, and revenue leakage analysis.
Another term teams mishandle is medical necessity. Many staff hear it and think it is just a coder problem. It is not. It is a claims management problem because payment depends on proving that the documentation, diagnosis selection, and service level support the billed service under payer rules. A claim can be technically accurate and still fail if the documentation does not justify the service intensity, site of care, frequency, or ordering requirements. That is why medical necessity criteria, clinical documentation improvement terms, Medicare documentation requirements, and essential guidelines for accurate clinical documentation belong inside your claims vocabulary, not off to the side in a separate compliance binder.
You also need to understand coordination of benefits, secondary billing, and patient liability allocation at a deeper level than basic definitions. COB errors do not just delay claims. They create duplicate billing, refund risk, patient complaints, and cross-payer confusion that can take weeks to unwind. Likewise, patient responsibility is not simply what remains after insurance. It is what remains after correct sequencing, correct adjudication, correct contractual application, and correct posting. That is why teams working high-value claims should consistently use coordination of benefits definitions, EOB interpretation guidance, patient balance terminology, and ethical billing practices to avoid shifting payer mistakes onto patients.
Quick Poll: What is your biggest claims management pain right now?
4. Terms That Help You Work Denials, Appeals, and Underpayments Intelligently
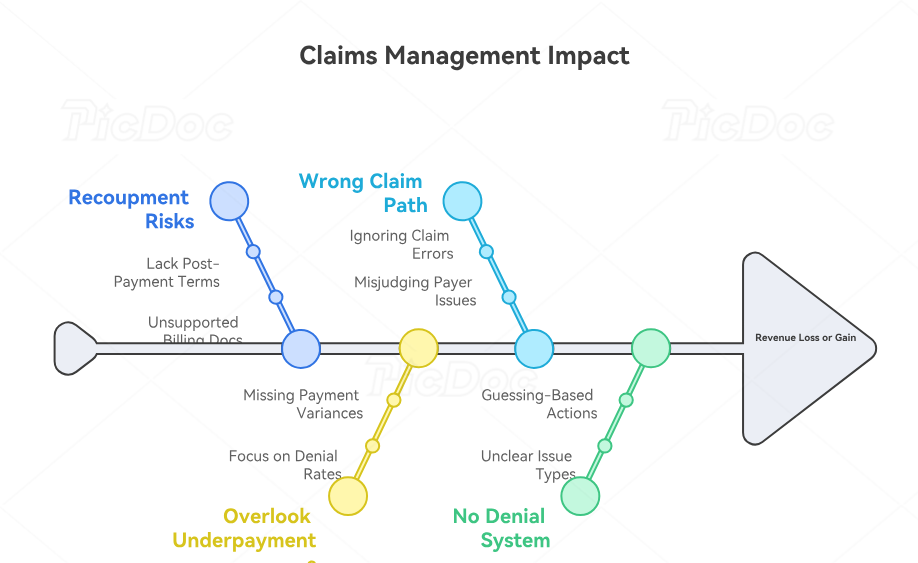
The most expensive claims teams are the ones that work denials without a denial language system. They open an EOB, see a code, make a guess, and send a rebill or appeal without clearly distinguishing documentation issues, registration issues, authorization issues, coverage exclusions, bundling issues, medical necessity issues, or payer processing errors. That creates motion without recovery. Strong teams use CARCs, insurance claim adjustment code guidance, RARCs, and coding denials management best practices to translate payer language into operational action.
One of the most important judgment calls in claims management is deciding between a corrected claim, a reconsideration, and a formal appeal. If the original claim itself was wrong, such as a missing modifier, wrong units, or incorrect frequency code, a corrected claim is often the right path. If the payer processed the claim incorrectly despite accurate billing, a reconsideration or appeal may be stronger. If supporting documentation was never submitted or was insufficiently matched to the issue, the appeal must be built around evidence, not frustration. Teams that do not understand those distinctions waste filing windows and bury staff in unnecessary touchpoints. This is where denials prevention and management, medical coding audits, audit term dictionaries, and medical billing compliance principles become recovery tools, not academic references.
Do not overlook underpayments just because the claim was technically paid. A partial payment can hide contract misconfiguration, multiple procedure reduction errors, incorrect out-of-network handling, inconsistent modifier recognition, or payer automation failures. Many organizations obsess over denial rates while losing more money through quiet underpayment patterns that no one owns. Underpayment recovery requires a stronger vocabulary around expected reimbursement, remit interpretation, variance logic, and payer contract behavior. That is why teams serious about performance lean on payment posting management, revenue cycle benchmark reporting, impact of coding accuracy on hospital revenue, and revenue leakage insights.
Then there are recoupments and takebacks, which deserve far more attention than many teams give them. A payer pulling back already-paid funds can destroy month-end confidence because the loss shows up after cash was already counted. Claims management terms must therefore include not only denial prevention language, but also post-payment review language. Why was the claim vulnerable? Was the original billing unsupported? Was the documentation incomplete? Was there a COB problem? Was the payer wrong? Without this vocabulary, finance sees noise instead of signal. With it, operations can use compliance audit trend reporting, billing compliance violation analysis, HIPAA compliance in billing, and ethical practices in medical billing to defend both revenue and credibility.
5. Terms That Separate Reactive Billing Teams From High-Performance Claims Operations
If you want to know whether a claims department is strategic or merely busy, look at the metrics language it uses. Reactive teams talk about volume, backlog, and “working accounts.” Strong teams talk about first-pass resolution rate, denial rate by root cause, A/R aging by payer, net collection rate, rejection turnaround time, appeal overturn rate, underpayment yield, and charge lag. Those terms force accountability because they expose where cash is getting trapped. That is why revenue cycle metrics and KPI definitions, RCM efficiency benchmarks, coding productivity benchmarks, and mastering revenue cycle management matter far beyond reporting dashboards.
Another separator is how the team defines ownership. In weak operations, every unresolved claim belongs to everyone and therefore to no one. In strong operations, every term maps to an accountable function. Eligibility belongs to front-end access. Charge capture belongs to the clinical-revenue interface. Documentation integrity belongs to provider education plus CDI. Modifier failures belong to coding review. Rejections belong to rapid correction teams. Underpayments belong to contract variance review. Denials belong to root-cause governance, not endless individual heroics. These distinctions become sharper when teams standardize around medical coding workflow terms, practice management system terminology, RCM software terms, and medical claims submission controls.
High-performance teams also use claims management language to improve upstream decision-making, not just back-end cleanup. If an authorization denial trend rises, they do not just appeal harder. They redesign scheduling checkpoints. If modifier denials spike, they do not just retrain billers. They audit documentation patterns and specialty templates. If patient balances rise unexpectedly, they do not just blame collections. They examine benefit estimation, COB accuracy, and posting logic. That approach depends on linking clinical documentation integrity, medical necessity guidance, EHR coding terms, accurate reimbursement strategy, and revenue leakage prevention into one operating model.
The final mindset shift is this: claims management is not about fighting the payer one claim at a time. It is about building a system where clean claims move fast, risky claims are identified early, denials are classified correctly, underpayments are visible, and compliance is built into the workflow instead of added later as fear-driven cleanup. The teams that win do not just learn terminology from a healthcare billing acronyms guide or a career roadmap in billing and coding. They turn that language into disciplined execution that protects margin, reduces staff burnout, and gives leadership a truthful picture of the revenue cycle.
6. FAQs About Healthcare Claims Management Terms
-
A rejected claim fails before payer adjudication, usually because of invalid or incomplete data such as subscriber information, NPI mismatches, missing modifiers, or format errors. A denied claim enters adjudication and is then refused fully or partially based on payer logic, policy, or documentation issues. That distinction matters because the workflow is different. Rejections require correction and rapid resubmission. Denials require analysis using clearinghouse terminology, CARCs, RARCs, and your denials management framework.
-
A clean claim is not simply a claim with codes on it. It is a claim that is complete, accurate, supported, payer-ready, and unlikely to require manual correction or payer clarification. Operationally, that means demographic data is correct, eligibility is verified, authorization is handled if needed, coding is accurate, documentation supports medical necessity, and payer edits have already been addressed. Teams improve clean-claim performance when they connect charge capture discipline, coding edit logic, clinical documentation quality, and the claims submission process.
-
Because they convert vague payer outcomes into actionable categories. A denial without structured CARC and RARC interpretation becomes guesswork. With them, you can identify whether the issue relates to medical necessity, authorization, bundling, eligibility, non-covered services, benefit exhaustion, or payer processing error. Once those codes are mapped correctly, you can assign ownership, standardize appeals, and fix root causes upstream. This is why teams pair claim adjustment reason code training, remark code interpretation, payment posting controls, and audit-ready billing compliance.
-
Submit a corrected claim when the original claim itself was materially wrong and the payer expects rebilling rather than dispute review. Typical examples include wrong units, wrong modifier use, corrected diagnosis sequencing, incorrect claim frequency coding, or missing claim-level data. File an appeal when the original claim was substantively correct but the payer’s denial or reduction was incorrect. Confusing those paths wastes time and can trigger filing-limit loss. Strong teams use denials prevention workflows, medical coding audit methods, and accurate reimbursement review to choose the right path quickly.
-
An underpayment is a payment that is lower than what should have been paid under payer contract terms, fee schedule logic, or expected reimbursement rules. Organizations miss underpayments because staff often equate “paid” with “correct.” Fast posting without expected-versus-actual comparison lets quiet revenue loss accumulate across high-volume claims. Underpayment control requires expertise in Medicare reimbursement, physician fee schedules, commercial insurance billing, revenue cycle KPI analysis, and revenue leakage insights.
-
New billers should master these terms early: clean claim, rejection, denial, eligibility, authorization, medical necessity, charge capture, claim scrubber, adjudication, allowed amount, contractual adjustment, patient responsibility, COB, CARC, RARC, corrected claim, appeal, payment posting, timely filing, A/R days, and net collection rate. That set gives a new biller a usable mental model of how a claim is created, processed, paid, reduced, or lost. To build depth fast, they should study healthcare billing acronyms, medical coding workflow terms, RCM terminology, and career-focused billing strategy guides.
-
Because unclear language creates duplicate work, blame-shifting, and bad prioritization. When teams do not distinguish rejections from denials, or contractual adjustments from collectible balances, staff work the wrong accounts and feel overwhelmed without producing results. A shared vocabulary makes routing cleaner, ownership sharper, training faster, and productivity more honest. That is why the smartest departments combine workflow terms, RCM software understanding, practice management system terms, and operational benchmark reporting into everyday management language.
-
Standardize definitions, then attach each definition to one control point and one owner. Build daily rejection correction, weekly denial root-cause review, monthly underpayment variance review, and tightly defined timely filing escalation. In other words, improve the language system before you add more labor to a broken process. Organizations usually recover more value by tightening claims submission workflows, denials prevention, payment posting management, and revenue leakage prevention than by throwing more people at unresolved ambiguity.