Guide to Utilization Review & Management Terms for Coders
Utilization review and utilization management are where clinical necessity, payer logic, documentation quality, and reimbursement pressure collide. For coders, these terms are not “someone else’s department.” They shape whether a stay is justified, whether a service level is defensible, whether documentation supports medical necessity, and whether the claim survives payer scrutiny. When coders do not understand UR and UM language, they code into a fog. When they do, they protect clean claims, reduce rework, strengthen appeals, and support revenue integrity with far more precision.
This guide is built to function as a working dictionary, not filler content. It explains the UR and UM terms coders keep running into, why they matter operationally, where teams get burned, and how to use the language to improve documentation, denials prevention, and payment defense. If your team already studies medical necessity criteria, revenue cycle management terms, denials prevention and management, Medicare documentation requirements, and guide to accurate medical billing and reimbursement, this article will connect those disciplines directly to utilization language coders must understand.
1. Why Utilization Review and Utilization Management Terms Matter to Coders
Coders often inherit the consequences of UR and UM decisions without being invited into the conversation early enough. A chart is coded after discharge, but the financial fate of that account may already have been shaped by admission status decisions, medical necessity screening, observation-versus-inpatient confusion, level-of-care disputes, prior authorization failures, and payer downgrades. That is why coders who understand utilization language work smarter than coders who only assign codes. They can recognize when documentation does not support the billed intensity, when the clinical story is weak for payer review, and when a denial is likely before it ever posts.
At a practical level, utilization review is the structured evaluation of whether services are medically necessary, appropriate in setting, efficient in duration, and supported by documentation. Utilization management is the broader administrative and clinical framework used to guide that review, control resource use, and align care with payer rules and evidence-based criteria. For coders, that means UR and UM terms are tied directly to clinical documentation improvement, coding audits, medical claims submission, revenue leakage prevention, and claim adjustment reason codes.
The pain point is not that coders need to become case managers. The pain point is that coders are often asked to defend coded services after the fact when the chart never clearly proved why the service belonged in that setting, at that intensity, for that duration. A coder may assign diagnosis and procedure codes correctly and still watch the claim unravel because the chart did not support inpatient level of care, because continued stay criteria were weak, or because the payer judged the service avoidable or misaligned with authorization. That kind of breakdown is rarely just a coding problem. It is a cross-functional failure touching medical record retention and storage terms, electronic medical record documentation terms, complete reference for coding query process terms, clinical documentation improvement dictionary terms, and medical coding workflow terms.
Strong coders use UR/UM vocabulary for three reasons. First, it helps them identify documentation gaps before claims go out. Second, it improves communication with CDI, case management, physicians, and denials teams. Third, it strengthens appeals because the coder can align coded facts with utilization logic instead of arguing in generic reimbursement language. When those teams share the same vocabulary, fewer accounts get trapped in expensive loops of rebilling, appeal writing, and payer back-and-forth visible later in revenue cycle metrics and KPIs, remittance advice remark codes, EOB interpretation, commercial insurance billing terms, and understanding coordination of benefits.
2. Core Utilization Review and Management Terms Every Coder Should Know
A coder does not need to memorize every acronym used by case management, but there is a core vocabulary that changes how records are read and how denials are anticipated. Start with medical necessity, because nearly every UR and UM dispute eventually comes back to it. Medical necessity is not just “the patient was sick.” It is whether the documented condition, risk, intensity of service, and setting were appropriate under payer rules and accepted standards. That makes it inseparable from medical necessity criteria, physician fee schedule terms, reference understanding Medicare reimbursement, guide to medical coding regulatory compliance, and understanding coding edits and modifiers.
Next comes level of care. This term answers a payer question coders ignore at their own risk: Was the patient treated in the right setting? A correct diagnosis code does not prove the need for inpatient care. A correct procedure code does not prove the service required a hospital rather than outpatient setting. If the note does not capture failed outpatient management, active monitoring needs, clinical instability, or treatment intensity, the coder may be right in code assignment but still lose the revenue argument. That is why level-of-care awareness strengthens SOAP notes and coding, problem lists in documentation, EHR coding terms, clinical documentation improvement, and accurate clinical documentation guidelines.
Two more critical terms are severity of illness and intensity of service. Severity of illness explains how sick the patient is; intensity of service explains how much care the patient actually required. Payers often want both dimensions to align. A patient may have significant chronic disease burden but not need acute inpatient services. Another patient may need aggressive monitoring and repeated interventions even if the final diagnosis looks deceptively simple on paper. Coders who understand that distinction are far better at identifying where the chart under-tells the case. They are also better at defending claims through coding audits, medical coding audit terms, revenue cycle efficiency benchmarks, coding productivity benchmarks, and impact of coding accuracy on hospital revenue.
Then there are the review types: prospective review, concurrent review, and retrospective review. Prospective review happens before service, often around authorization. Concurrent review happens during treatment and shapes approved days and continued stay decisions. Retrospective review happens after the fact, when weak documentation gets exposed without mercy. Coders who ignore these distinctions often misread why denials occurred. The payer may not be disputing the code itself; it may be disputing whether the service should have happened in that way, at that time, in that setting, for that duration. Understanding this helps coders work more intelligently with payment posting and management, claim adjustment reason codes, RARC interpretation, clearinghouse terminology, and medical billing practice management systems.
3. How UR and UM Terms Affect Coding Accuracy, Claim Defense, and Reimbursement
The biggest mistake organizations make is treating utilization language as separate from coding language. In real revenue cycle work, they overlap constantly. A coder may not choose the admission status, but the coded claim still becomes the object the payer evaluates. If the record supports diagnoses but not the need for inpatient admission, payment may collapse. If procedures are coded correctly but prior authorization does not match the service delivered, the account still becomes a billing problem. If the chart captures illness but not active treatment intensity, continued-stay denials become easier for payers to issue and harder for hospitals to reverse.
This is why UR and UM literacy matters most in three operational zones. The first is status-sensitive accounts such as inpatient versus observation disputes. These accounts burn time because the payer often agrees the patient needed care but argues the care belonged in a lower-cost setting. Coders who understand the language of observation, inpatient, admission criteria, and Condition Code 44 can flag risk earlier and communicate more effectively with utilization teams. That reduces downstream chaos in Medicare reimbursement interpretation, healthcare cost reporting essentials, understanding cost reporting in medical billing, value-based care coding terms, and accountable care organization billing terms.
The second zone is medical necessity denials. These are among the most frustrating denials because the coding may be technically correct while the payment rationale still fails. A payer may say the service was not necessary, not at that frequency, not in that setting, or not supported by the record. Coders who understand utilization language do not respond with generic statements. They build defenses around documented severity, failed conservative treatment, monitoring intensity, intervention complexity, risk of deterioration, and progression of care. That makes their contributions far more useful in coding denials management, comprehensive guide to denials prevention, medical coding error rates, revenue leakage analysis, and compliance audit trends.
The third zone is documentation integrity. Utilization review constantly exposes the same weakness: providers document events, but not always the rationale that proves necessity and setting. A note may show labs, meds, and monitoring, yet fail to explain why the patient could not safely be treated elsewhere. A coder who understands UR terminology reads that chart differently. Instead of seeing only codeable diagnoses, that coder sees the missing argument. This is why strong organizations connect coders with coding query process terms, EMR documentation terms, electronic health record integration terms, encoder software terms, and medical coding automation terms.
Quick Poll: What is your biggest utilization review pain point right now?
4. High-Risk Utilization Review Scenarios Coders Need to Recognize Early
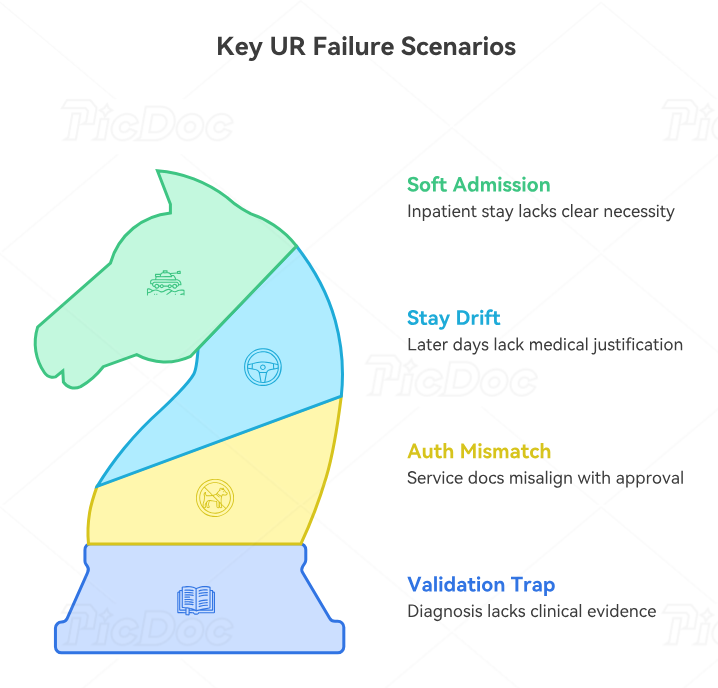
One of the most expensive UR failures is the soft admission: a patient is admitted inpatient, but the record reads like extended monitoring rather than clearly necessary acute hospitalization. There may be symptoms, tests, and caution, but not enough documented instability, treatment intensity, or risk. The coder assigns real diagnoses, the claim goes out, and then the payer downgrades the stay. At that point, the organization is not fighting about code accuracy alone. It is fighting about the clinical story told by the chart. This is where coders who understand utilization language can flag risk earlier and support cleaner communication with clinical documentation integrity, problem-list documentation, medical necessity guidance, accurate reimbursement practices, and revenue cycle KPIs.
Another high-risk scenario is the continued-stay drift. The admission may have been justified on day one, but later hospital days become hard to defend. Testing is done, active treatment slows, and the patient remains for placement, discharge planning, or nonclinical delays. If the chart does not clearly separate medical need from operational delay, payers can deny those extra days. Coders who understand terms like avoidable day, discharge planning delay, and continued-stay review read these records with more skepticism and precision. They know where the argument weakens and can help denials teams build more accurate appeals using medical record retention terms, EOB guidance, CARCs, RARCs, and medical coding audit terms.
A third scenario is the authorization mismatch. The payer may approve a service, but the documented diagnosis, procedure details, timing, or setting do not line up with what was authorized. Coders often see the damage later as a denial and may be asked to “fix” it from the back end. But authorization failures are usually upstream control failures, not downstream coding tricks. The coder’s job becomes easier when organizations align charge capture, scheduling, authorization, and final code assignment through charge capture terms, medical billing software selection, revenue cycle management software terms, practice management system terms, and ethical billing practices.
Finally, there is the clinical validation trap. A diagnosis may be documented, but if the clinical evidence is weak, both medical necessity and severity arguments weaken with it. Coders should not treat diagnosis assignment as a detached mechanical act. In utilization disputes, clinical credibility matters. Strong coding teams know when a record supports the diagnosis robustly and when it merely labels the patient without enough indicators. That awareness strengthens compliance in medical coding, understanding medical coding audits, top coding error prevention, coding compliance trends, and billing compliance violations and penalties.
5. Best Practices for Coders Using Utilization Review and Management Language
The first best practice is simple but powerful: read the chart for necessity, not just codeability. Many coders are trained to hunt diagnoses, procedures, complications, comorbidities, and sequencing clues. They should also be trained to ask: Does this record prove why this service belonged here? That shift changes everything. It improves query quality, catches weak records earlier, and reduces surprise denials. Teams that adopt this mindset often perform better in medical coding workflows, coding education and training, CEU development, career development guidance, and certification exam terms.
The second best practice is build shared language with CDI, UM, and denials teams. If coders talk in code sets while utilization staff talk in criteria tools and denials staff talk in payer letters, the organization creates translation delays that waste money. Shared terminology around medical necessity, level of care, severity, intensity, observation, status downgrade, and clinical validation reduces friction and makes appeals sharper. The most resilient teams treat utilization terminology as a common operating language, not a departmental dialect. That approach also strengthens work in revenue cycle metrics, revenue cycle efficiency, mastering revenue cycle management, future innovations in billing software, and predictive analytics in medical billing.
The third best practice is audit utilization-sensitive denials by pattern. Do not just count denials. Segment them by status downgrade, medical necessity, authorization mismatch, continued-stay failure, and clinical validation. Then look by payer, service line, and provider pattern. This makes coder education more surgical and far more effective than generic compliance lectures. It also reveals whether the true issue is weak provider narrative, weak front-end controls, inconsistent query escalation, or poor payer-specific rule management. Those insights are much more valuable than broad denial tallies and feed directly into coding workforce improvement, productivity benchmarking, error-rate control, impact of regulations on billing, and upcoming regulatory changes affecting billing.
The fourth best practice is treat documentation queries as prevention tools, not rescue tools. If coders only query after a claim is already in danger, the organization stays in reactive mode. Better organizations use UR/UM knowledge to refine documentation templates, admission note expectations, continued-stay language, and discharge summaries. When providers document necessity better the first time, coders code faster, denials teams appeal less, and reimbursement becomes less volatile. That discipline scales especially well when paired with medical coding automation terms, AI in revenue cycle management, future skills for medical coders, the future of medical coding with AI, and automation transforming billing roles.
6. FAQs About Utilization Review and Management Terms for Coders
-
Utilization review is the specific assessment of whether care was necessary, appropriate, and delivered in the right setting and duration. Utilization management is the broader system of policies, reviews, authorizations, and controls used to manage that process. Coders need both concepts because they shape medical necessity, status decisions, and payer denials tied to revenue cycle management terms and regulatory compliance.
-
Because the coded claim still lives or dies based on whether the record supports the setting. Coders who understand inpatient, observation, and continued-stay logic can spot weak narratives early and help protect reimbursement through better queries, stronger documentation, and smarter appeals grounded in medical necessity guidance and accurate reimbursement practices.
-
The highest-value terms are medical necessity, level of care, inpatient admission, observation status, severity of illness, intensity of service, continued-stay review, avoidable day, status downgrade, and clinical validation. These terms directly affect how inpatient accounts survive payer scrutiny and how coders collaborate with CDI teams and audit teams.
-
They help coders explain not just what was coded, but why the service was justified in that setting, at that intensity, for that duration. That makes appeals more precise and much harder for payers to dismiss. Strong appeals usually combine coded facts, clinical indicators, treatment intensity, and payer logic visible in CARCs, RARCs, and denials management analysis.
-
The biggest weakness is failing to explain why the patient required that specific setting and intensity of care. Charts often show events and interventions without clearly stating risk, failed lower-level options, or the reason continued hospitalization remained necessary. That gap undermines otherwise valid coding and makes clinical documentation improvement, SOAP notes, and problem-list accuracy far more important than many teams realize.
-
It can, but only if documentation, payer rules, and internal workflows are already disciplined. Automation can flag mismatches faster, but it also scales weak logic faster when the foundation is poor. Coders who want to stay valuable should understand both utilization language and the future of tech-enabled coding through AI in revenue cycle management, future skills for coders, coding automation terms, and future-proof medical coding careers.