Medical Abbreviations & Acronyms Dictionary for Coders
A coder can lose accuracy long before the code book opens. The damage often starts when a short note, copied phrase, specialty shorthand, or payer acronym gets read too quickly inside the EHR documentation workflow, the medical coding workflow, the CDI review process, or the coding query process. Clinical abbreviations are widespread in health records, and research has long shown that many are ambiguous in context.
This dictionary is built for coders who need speed without sloppiness. It explains the abbreviations and acronyms that shape claim accuracy, audit readiness, medical necessity review, and revenue leakage prevention so you can read chart language the way high-level coding teams do: fast, skeptical, contextual, and defensible.
1. Why Abbreviation Mastery Is a Revenue Skill, Not Just a Reading Skill
Medical abbreviations look harmless because they save time for the documenting clinician, but for coders they can create three separate problems at once: meaning drift, specialty drift, and payment drift. Meaning drift happens when one abbreviation can point to multiple concepts. Specialty drift happens when the same shorthand means one thing in radiology coding, another in behavioral health billing, and something else in home health coding. Payment drift happens when the wrong expansion of a term infects charge capture, claims management, reimbursement, and later claims reconciliation. Research and official safety guidance both support the idea that abbreviation ambiguity is common enough to require deliberate controls.
This is why advanced coders do not “decode” abbreviations in isolation. They triangulate them against the SOAP note structure, the problem list, the EHR coding context, the query policy, and the medical record retention standard. If “MS” appears, they do not rush. They ask whether the encounter context supports multiple sclerosis, mitral stenosis, morphine sulfate, or magnesium sulfate. The coder who moves too fast converts shorthand into fiction, and fiction does not survive audits.
The danger is even higher because modern records are dense. CMS describes the EHR as a longitudinal record that can include progress notes, problems, medications, vital signs, history, immunizations, labs, and radiology data. That means abbreviations do not appear in one neat spot; they appear across orders, assessments, templates, import fields, and scanned records. A coder who wants defensible abstraction has to read abbreviations through HIM governance, encoder software logic, coding automation oversight, and EHR integration controls, not just memory.
| Abbreviation / Acronym | What It Means | Where Coders See It | Why It Can Mislead | Best Coder Action |
|---|---|---|---|---|
| H&P | History and Physical | Admission and pre-op documentation | May be copied forward and not reflect current status | Check date, author, and update notes |
| CC | Chief Complaint | ED and office notes | Can be symptom-only and not final diagnostic support | Use with HPI and assessment, not alone |
| HPI | History of Present Illness | Provider narrative | May include ruled-out or questioned conditions | Separate symptoms, possibilities, and confirmed findings |
| ROS | Review of Systems | Clinic and hospital notes | Negative symptom review is not the same as a diagnosis | Use it to clarify, not to overcode |
| PE | Physical Exam | All encounter types | Abnormal findings may conflict with assessment | Reconcile with plan and final impression |
| Dx | Diagnosis | Assessments, superbills, problem lists | Sometimes used loosely for possible conditions | Confirm documentation certainty level |
| Tx | Treatment or therapy | Plans and consults | Can reference prior care, not today’s service | Tie it to date of service |
| Hx | History | PMH, PSH, FH, SH sections | Past conditions may look active if read fast | Separate historical from current conditions |
| PMH | Past Medical History | Histories and intake forms | Imported PMH may be inaccurate or stale | Cross-check with active assessment |
| PSH | Past Surgical History | History sections | Prior procedures can be confused with current services | Verify current encounter procedure separately |
| FH | Family History | Preventive and risk notes | Family disease does not equal patient diagnosis | Code history status only when supported and reportable |
| SH | Social History | Primary care and behavioral notes | Substance, housing, or work context affects specificity | Use it to sharpen context, not invent diagnoses |
| SOB | Shortness of Breath | ED, pulmonology, hospitalist notes | Symptom may coexist with many confirmed diagnoses | Look for final cause and coding setting rules |
| DOE | Dyspnea on Exertion | Cardiology and pulmonary notes | Can be symptom-only or part of chronic disease picture | Use assessment and plan to decide significance |
| CP | Chest Pain | ED and observation records | May later be ruled to GERD, angina, or noncardiac pain | Follow diagnostic evolution across the stay |
| N/V | Nausea and Vomiting | ED, GI, oncology | Often documented as a symptom cluster only | Check whether cause or complication is finalized |
| LOC | Loss of Consciousness or Level of Consciousness | Trauma and neuro notes | Context changes meaning completely | Read surrounding sentences and specialty context |
| R/O | Rule Out | ED differentials and consults | Not a confirmed diagnosis in many coding settings | Follow setting-specific coding rules |
| s/p | Status Post | Post-op and follow-up notes | May refer to remote history, not current complication | Confirm timing and relevance to visit |
| PRN | As Needed | Medication and nursing instructions | Useful clinically, but not always code-driving | Do not overread it into a billable condition |
| DME | Durable Medical Equipment | Orders, discharge planning, claims | Often triggers payer-specific documentation standards | Check coverage and necessity support |
| DOS | Date of Service | Claims, charge review, remits | Mismatches create denials and audit noise | Match note date, order date, and billed date carefully |
| NPI | National Provider Identifier | Enrollment, claims, payer setups | Wrong NPI can corrupt billing and attribution | Validate rendering, billing, and referring roles |
| TIN | Taxpayer Identification Number | Payer enrollment and group billing | Entity mismatch can cause claim rejection or payment delay | Align payer file and claim submission logic |
| EOB | Explanation of Benefits | Patient and payer payment review | Can be confused with ERA or remittance data | Use for adjudication clues, not just patient balance |
| COB | Coordination of Benefits | Multi-payer accounts | Incorrect sequencing drives preventable denials | Confirm primary, secondary, and filing order rules |
| CARC | Claim Adjustment Reason Code | Remittance review | Can be misread without remark code context | Pair with RARC and claim facts |
| RARC | Remittance Advice Remark Code | Remittance review | Adds nuance often missed in denial root-cause review | Read with CARC, policy, and documentation |
| LCD | Local Coverage Determination | Medicare coverage review | Coverage may vary by contractor and documentation specifics | Check the relevant MAC policy before coding assumptions |
| NCD | National Coverage Determination | Medicare policy review | Can override casual office assumptions | Tie coding to national coverage language when applicable |
| ABN | Advance Beneficiary Notice | Medicare patient financial liability workflow | Documentation timing matters, not just form presence | Check notice validity and timing before balance transfer |
| RCM | Revenue Cycle Management | Operations and reporting | Teams treat it like finance only, but coding drives it | Link abbreviation clarity to revenue outcomes |
| HCC | Hierarchical Condition Category | Risk adjustment documentation | Problem list carry-forward can mimic active disease | Validate present assessment and treatment support |
2. The Clinical Documentation Abbreviations That Decide Whether You Can Trust a Note
The first group coders need to master lives in chart narrative, not on the claim form. Terms like H&P, HPI, ROS, PE, PMH, PSH, FH, and SH look foundational, but each one carries a hidden trap. H&P may be stale. HPI may contain differential language that never became a final diagnosis. ROS may document negatives that help medical necessity but do not independently support reportable conditions. FH and SH often explain risk, exposure, or background, but they do not magically convert family disease or lifestyle factors into active patient diagnoses. This is where CDI terms, problem list guidance, SOAP note interpretation, and medical necessity criteria have to work together.
A stronger coder reads abbreviations by asking three questions in order. First, where in the record is this abbreviation appearing: history, assessment, plan, order, nursing note, test impression, or billing field? Second, what service line owns the note: lab and pathology, radiology, telemedicine, or sleep medicine? Third, did the provider finalize the concept or merely mention it? Those questions stop coders from turning abbreviations into unsupported specificity.
The abbreviation itself is rarely the whole story. “s/p CABG,” “r/o PE,” “hx CHF,” and “DOE x 2 weeks” do not all behave the same way in coding logic. One points to postoperative status, one to uncertainty, one to history, and one to symptom duration. If your team does not train coders to separate current disease from historical disease, confirmed disease from suspected disease, and symptom from cause, your coding audit results, denial management, claims correction work, and revenue leakage rate will reflect it.
3. The Payer, Billing, and Remittance Acronyms That Quietly Shape Revenue
Some coders know clinical shorthand well but still get trapped by payer acronyms that control whether clean documentation becomes clean payment. EOB, COB, CARC, RARC, LCD, NCD, ABN, DOS, NPI, and TIN are not back-office trivia. They are the difference between understanding adjudication and guessing at it. When teams misread these acronyms, they create bad appeals, misroute balances, misclassify denials, and miss the real root cause. That is why serious coders need fluency in healthcare billing acronyms, claims adjustment reason codes, remittance advice remark codes, and coordination of benefits. Local Coverage Determinations are current Medicare contractor policies defined by CMS, which is exactly why teams cannot treat them as stale trivia.
Take EOB and ERA-style thinking as an example. An inexperienced reviewer sees nonpayment and assumes coding failed. A better reviewer asks whether payer sequencing failed, whether the modifier logic failed, whether CMS-1500 fielding or UB-04 logic failed, whether clearinghouse edits fired first, or whether the record failed a coverage policy tied to medical necessity. That level of acronym fluency saves time in payment posting, claims management, accurate reimbursement review, and RCM metrics analysis.
The same applies to coverage acronyms. If a coder sees DME, HCC, MIPS, ACO, or MACRA without understanding how those concepts touch documentation, reimbursement, and reporting, the chart can be coded correctly at the code-set level and still underperform operationally. That is why coders should connect abbreviation knowledge with risk adjustment coding, HCC definitions, value-based care terminology, and MACRA and MIPS concepts instead of treating those acronyms as somebody else’s department.
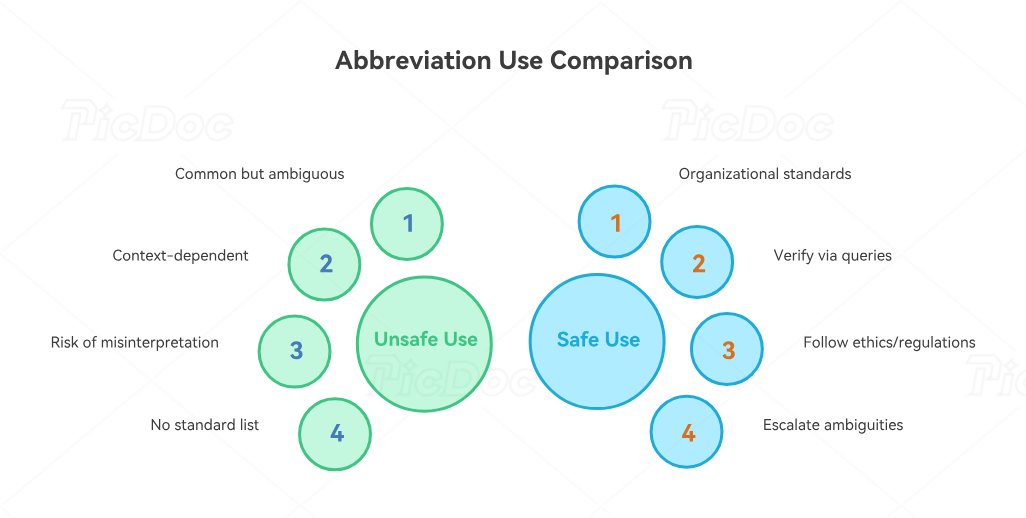
4. The Abbreviations Smart Coders Slow Down For on Purpose
The most dangerous abbreviations are not always rare. They are often the common ones that look familiar enough to bypass caution. “MS” can mean multiple sclerosis, morphine sulfate, magnesium sulfate, or mitral stenosis depending on context. “CP” might be chest pain, cerebral palsy, or chest pressure shorthand in a loosely written note. “PT” can indicate patient, prothrombin time, physical therapy, or a therapy service line. Research on clinical abbreviation ambiguity repeatedly shows that nonstandard and context-dependent abbreviations are a real interpretation hazard, which is why speed alone is not professionalism.
This is where internal controls matter more than memory. Joint Commission guidance is clear that it does not publish a universal approved list of abbreviations, and its safety framework continues to emphasize reducing error from ambiguous shorthand and unsafe symbols. That means each organization needs its own disciplined standard for what abbreviations are acceptable, what terms require expansion, and what documentation requires clarification before coding. Coders should work with coding ethics and standards, regulatory compliance guidance, documentation requirements for coders, and coding education terms instead of relying on hallway folklore.
A mature coder also knows when abbreviation interpretation becomes a query issue. If an abbreviation could reasonably support more than one clinically plausible diagnosis, if it conflicts with the assessment, if it appears only in a copied list, or if it is the only place a potentially reportable condition appears, that is not the moment to guess. It is the moment to pause, verify, and escalate through the coding query process, the medical coding audit framework, the medical billing compliance workflow, and the documentation improvement model. That pause protects both code accuracy and organizational credibility.
5. How to Build a Coder-Safe Abbreviation Policy That Actually Works
The strongest abbreviation policy is not a giant list nobody reads. It is a workflow tool embedded in real production. Start by building one internal dictionary divided into four lanes: clinical documentation abbreviations, specialty abbreviations, payer and remittance acronyms, and prohibited or escalation-only abbreviations. Then tie each term to example contexts and a clear coder action: trust, verify, query, or do not code from this alone. That single framework works far better when it is linked to your encoder software, practice management system, RCM software stack, and coding automation tools.
Next, train by failure pattern, not by alphabet. Organize examples around the mistakes that actually cost money: symptom mistaken for diagnosis, history mistaken for active disease, rule-out mistaken for confirmed disease, specialty shorthand mistaken across service lines, and remittance acronyms misunderstood during follow-up. Use real cases from coding denials analysis, revenue leakage reviews, payment posting findings, and medical billing reconciliation work. People remember pain better than vocabulary drills.
Finally, monitor abbreviation risk like any other quality signal. Track query rates triggered by ambiguous shorthand, denial rates tied to documentation interpretation, overturn rates on audited charts, and the specialties that generate the most nonstandard abbreviations. Fold that data into revenue cycle KPIs, coding productivity benchmarks, workforce training plans, and career development for coders. If leadership only measures speed, abbreviations will stay dangerous. If leadership measures defensible speed, abbreviation quality improves fast.
6. FAQs About Medical Abbreviations & Acronyms for Coders
-
No. A shorthand term may help point you toward the clinical concept, but it should be validated against the full note context, the final assessment, the care setting, and any applicable documentation requirements. The safer workflow is to combine the abbreviation with the problem list, the query process, and the medical coding audit lens, especially when the abbreviation is ambiguous. Clinical abbreviation ambiguity is a documented issue, not a theoretical one.
-
Any abbreviation with multiple common meanings should slow you down immediately. Terms like MS, CP, PT, LOC, and SOB can be interpreted correctly only when anchored to specialty, sentence context, and final assessment. Your organization should also maintain a practical “escalation terms” list inside its coding ethics and standards, regulatory compliance, and education framework.
-
They are absolutely the coder’s problem when they affect documentation sufficiency, claim structure, coverage logic, and denial root cause. A coder who understands EOBs, CARCs, RARCs, and COB sequencing writes cleaner appeals, spots documentation gaps sooner, and protects revenue faster.
-
Yes, but not as a dead policy file. Joint Commission makes clear it does not provide a universal approved list, which means organizations need their own controlled reference tied to documentation safety and operational reality. The best version lives inside EHR governance, HIM policy, coding workflow controls, and record retention practices.
-
Because copied language turns yesterday’s shorthand into today’s false certainty. A historical condition can look active, an old symptom can look current, and an outdated differential can survive into a new encounter if no one cleans it up. That is why coders need strong habits around problem list review, SOAP note interpretation, CDI collaboration, and EHR integration logic.
-
Read the abbreviation last, not first. Start with encounter type, specialty, assessment, and plan. Then ask whether the shorthand is confirmed, historical, symptomatic, uncertain, or operational. That habit makes you stronger in medical necessity review, claims management, audit preparation, and reimbursement accuracy.
-
They should learn them in clusters tied to work: admission note abbreviations, symptom abbreviations, surgery status abbreviations, remittance acronyms, and coverage acronyms. Then they should review them against real charts, denial cases, and query examples from coding education resources, credentialing pathways, CBCS terminology, and career roadmaps. Overconfidence grows when vocabulary is memorized without context.