Understanding Medical Coding System Updates & Releases
Medical coding does not break because coders forget definitions. It breaks when yearly, quarterly, and payer-specific updates quietly change the rules under active workflows while teams keep coding as if nothing moved. A deleted code, a revised inclusion note, a new modifier instruction, or a payer edit refresh can turn clean production into denials, rework, lost revenue, and audit exposure within days.
The professionals who stay ahead do not “watch for updates” casually. They build an operational habit around release calendars, documentation impact, edit testing, provider communication, and denial surveillance. That is how coding teams protect accuracy, reimbursement, and compliance at the same time.
1. Why Medical Coding System Updates Matter More Than Most Teams Realize
Medical coding system updates are not small administrative changes. They alter how diagnoses are represented, how procedures are reported, how medical necessity is evaluated, how payer edits fire, and how revenue moves across the revenue cycle. A team that ignores updates will eventually feel the damage in denials, retractions, payment delays, compliance findings, and physician frustration.
The first problem is timing. Many organizations assume updates only matter on the effective date. In practice, risk begins earlier. Teams need lead time to review official guidance, compare old and new language, identify high-volume services affected, update encoder logic, revise cheat sheets, retrain staff, and monitor production after go-live. Without that runway, coders are forced to learn in live claims, which is the most expensive classroom in revenue cycle operations.
The second problem is fragmentation. Coding updates do not arrive from a single source. ICD diagnosis updates, CPT and procedure reporting changes, payer policy revisions, National Correct Coding Initiative logic, fee schedule revisions, medical necessity requirements, and documentation rules can shift on different timelines. That is why strong teams pair coding review with a broader grasp of medical coding workflow terms, coding edits and modifiers, medical coding regulatory compliance, Medicare documentation requirements, and revenue cycle management terms.
The third problem is that updates rarely fail loudly at first. Instead, they leak money quietly. A new code may be missing from the chargemaster. A revised diagnosis description may not map correctly in the EHR. A payer may reject claims because coverage logic changed while documentation templates stayed the same. These are classic forms of revenue leakage prevention, and they often show up downstream in claims reconciliation, payment posting, claim adjustment reason codes, and remittance advice remark codes.
The strongest way to think about coding system releases is this: every update is both a coding event and an operational event. It changes code selection, but it also affects documentation, billing logic, edits, payer acceptance, appeal strategy, quality reporting, and productivity. Teams that treat releases as isolated coder education sessions stay reactive. Teams that treat them as system-wide implementation projects protect both compliance and cash flow.
| Update Area | What It Usually Changes | Why It Creates Risk | Best Practice Action |
|---|---|---|---|
| ICD code additions | New diagnostic specificity options | Teams keep using broader outdated choices | Refresh diagnosis preference lists and coder references |
| ICD code deletions | Retired diagnosis options | Claims reject or map incorrectly | Remove deleted codes from templates and encoder favorites |
| ICD description revisions | Changed wording or instructional notes | Coders misread scope of code use | Train on wording changes, not just code numbers |
| CPT new codes | Fresh procedure reporting options | Services remain reported with legacy combinations | Audit high-volume procedures for replacement opportunities |
| CPT deleted codes | Removed procedure selections | Charge capture continues using dead codes | Coordinate with chargemaster and front-end scheduling teams |
| CPT revised guidelines | New parenthetical or section instructions | Correct code used with wrong support rules | Build service-line teaching examples around changed notes |
| HCPCS Level II updates | Supply, drug, and non-physician service changes | Drug units and temporary codes get miscoded | Compare inventory, billing units, and payer guidance |
| Quarterly drug code releases | New J-codes and replacements | Manual crosswalks lag behind payer requirements | Review pharmacy and infusion workflows before effective date |
| NCCI edit refreshes | Bundling and modifier logic updates | Separately billable services get denied | Test top code pairs and retrain on valid modifier use |
| MUE changes | Unit limits update | Overstated units trigger denials or audits | Monitor high-unit departments and edit claims pre-bill |
| Fee schedule revisions | Relative values or payment rates shift | Leadership misses reimbursement impact | Model revenue effect by specialty and service mix |
| Coverage policy updates | Diagnosis or documentation requirements change | Clean-coded claims still fail medical necessity | Link coding education with payer policy review |
| LCD/NCD changes | Medicare coverage criteria shift | Documentation gaps block payment | Update provider prompts and diagnosis support lists |
| Modifier instruction updates | When modifiers are or are not allowed | Appeals fail because original modifier logic was weak | Teach modifier intent with real denial examples |
| E/M guideline changes | Selection method, time, or MDM rules shift | Provider note habits become misaligned | Run focused provider-coder alignment sessions |
| Telehealth policy updates | POS, modifier, or covered service changes | Claims mismatch payer-specific requirements | Maintain payer matrix for virtual care billing |
| Risk adjustment model updates | Diagnosis capture significance changes | Chronic burden goes underreported | Review high-value chronic conditions and suspecting workflows |
| HCC mapping changes | Diagnosis-to-risk relationships shift | Population revenue forecasts drift | Coordinate coding, analytics, and value-based teams |
| MACRA/MIPS measure changes | Quality and reporting logic updates | Documentation misses numerator opportunities | Translate reporting rules into coder and clinic workflows |
| Clearinghouse edit updates | Front-end data validation shifts | Rejections spike before payer adjudication | Review new rejection patterns daily after release |
| Payer companion guide changes | Submission and field requirements change | EDI files pass internally but fail externally | Update billing rules and test transmissions early |
| EDI transaction revisions | Data formatting expectations update | Claim data elements break in transmission | Involve IT, clearinghouse, and billing operations together |
| Encoder software updates | Logic, prompts, and references change | Coders trust outdated local workarounds | Validate vendor content against official guidance |
| EHR template revisions | Structured data capture changes | New codes lack the needed documentation fields | Map every coding change to note template impact |
| Problem list maintenance rules | Diagnosis carry-forward handling shifts | Inactive or unsupported diagnoses persist | Tighten clinician review and coder escalation rules |
| Documentation query policy changes | Clarification thresholds evolve | Teams either over-query or miss needed clarification | Recalibrate compliant query standards with examples |
| Medical necessity updates | Support criteria shift | Correct codes no longer guarantee payment | Crosswalk coverage criteria into coding education |
| Audit focus area changes | Regulators or payers target new error types | Legacy monitoring misses emerging exposure | Realign internal audits with new external scrutiny |
| Local policy bulletins | Regional billing instructions vary | National assumptions create local denials | Track payer-region exceptions in one control document |
| Internal charge master updates | Operational billing setup changes | Approved code changes never reach claim generation | Reconcile coding, charge capture, and billing system build |
2. The Main Coding Systems That Change and How Each Release Affects Daily Work
A coder who understands update mechanics works faster and makes safer decisions than a coder who only memorizes code sets. That begins with separating which system is changing and what type of impact to expect.
Diagnosis system updates affect condition specificity, manifestation reporting, sequencing rules, inclusion terms, excludes notes, and code validity. When diagnosis releases change, the downstream effect is often larger than teams expect because diagnosis coding touches medical necessity, risk capture, disease trending, and payer acceptance. Coders working with chronic disease documentation, specialty encounters, and complicated follow-up care should stay especially sharp with ICD-11 coding standards and best practices, medical necessity criteria, electronic health record coding terms, and problem lists in medical documentation.
Procedure system updates affect how services are reported, bundled, and valued. A new CPT code can replace an old reporting workaround. A revised CPT guideline can change whether an add-on code is appropriate. A deleted code can create immediate front-end and back-end confusion if scheduling, charge entry, and billing keep using it. That is why procedure releases need coordination with charge capture terms, physician fee schedule terms, guide to accurate medical billing and reimbursement, and specialty references like radiology coding or lab and pathology coding essentials.
HCPCS and drug-related updates create major risk in infusion, injection, DME, and supply-heavy environments. A unit definition error or late code replacement can lead to systematic underbilling or payer rejection across entire service lines. These environments need disciplined review tied to infusion and injection therapy billing terms, anesthesia coding and billing terms, ambulance and emergency transport coding, and commercial insurance billing terms.
Edit and policy updates are where many experienced coders get blindsided. The code itself may be correct, but the claim still fails due to modifier logic, frequency edits, payer policy changes, or documentation rules. That is why coders should pair code updates with clearinghouse terminology, EDI billing terms, medical billing practice management systems terms, and revenue cycle management software terms.
Value-based and reporting updates matter because coding increasingly affects more than claim payment. It influences quality scores, risk models, and performance adjustments. Teams that still think only in fee-for-service terms miss the growing relevance of value-based care coding terms, MACRA terms, MIPS guidance, HCC definitions, and risk adjustment coding.
The practical lesson is simple: do not ask only, “What changed?” Ask, “Which workflows, specialties, edits, templates, and payer rules does this change touch?” That second question is where operational maturity lives.
3. How to Build a Reliable Process for Tracking Coding Updates Without Missing Critical Changes
Most coding teams do not fail because they lack intelligence. They fail because their tracking process is informal. One person watches updates. One educator sends a summary email. One supervisor mentions a change in a meeting. Then production pressure takes over, the message fragments, and old habits remain active.
A reliable process starts with an update ownership model. Someone must own diagnosis releases. Someone must own procedure releases. Someone must own payer bulletins and edit behavior. Someone must own education deployment. Someone must own post-go-live monitoring. When no one owns each part, everyone assumes someone else did it.
Next, build a release calendar. Coders should know when annual code changes arrive, when quarterly updates are expected, when payer contracts or policy refreshes typically drop, and when internal system builds must be completed. Pair that with a standing review workflow connected to medical coding audit terms, coding ethics and standards, medical record retention and storage terms, and health information management terms.
Then create a change impact worksheet for every meaningful update. The worksheet should answer:
Which codes, guidelines, notes, edits, or policies changed?
Which specialties or departments are affected?
Which providers need education?
Which templates, order sets, or charge tools need revision?
Which payers are likely to deny if implementation is late?
Which denial codes or rejections should be watched after go-live?
Which audit samples should be pulled in the first two to four weeks?
This is where coders become strategic. They stop acting like code lookup staff and start acting like revenue protection professionals. Teams that connect updates to claims management terms, medical billing reconciliation terms, collections and bad debt concepts, and revenue cycle metrics and KPIs can actually prove the business value of good implementation.
Finally, require post-release validation. Training alone is not enough. Pull real claims. Review denials. Check edit hits. Compare coder patterns before and after the change. Audit whether providers are documenting the new distinctions correctly. This is where many teams discover the painful truth: they announced the update, but the old behavior stayed alive in the workflow.
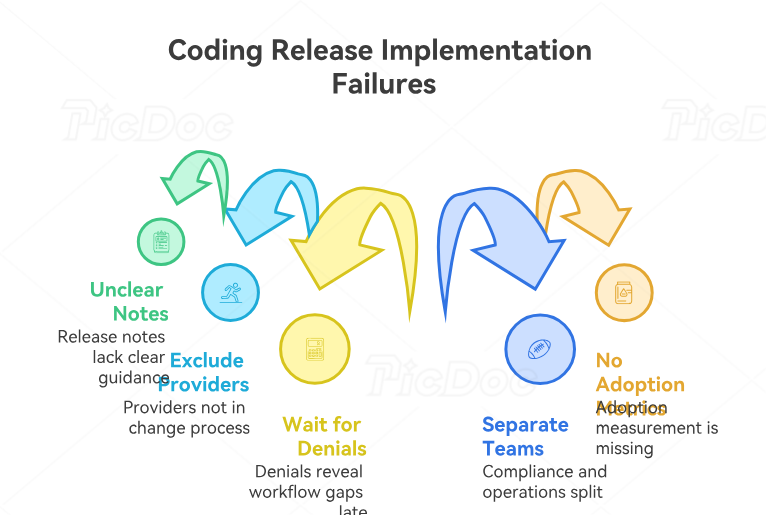
4. Where Coding Update Implementations Usually Fail and How to Prevent Expensive Mistakes
The first implementation failure is treating release notes as self-explanatory. They are not. Technical language does not automatically convert into clean chart-level decisions. Coders need scenario-based examples that show what changed, why prior logic is now risky, what documentation should support the new selection, and what denials are likely if the team misses the change. This is especially important when teams use encoder software, EHR integration terms, coding automation terms, and electronic medical record documentation terms.
The second failure is excluding providers from the change process. Coders may understand the new rule, but if documentation still reflects outdated habits, claims remain weak. A release that changes specificity requirements, procedure distinctions, or support criteria must be translated into physician-facing language. Providers do not need long manuals. They need concise instruction on what must now be documented differently, what phrases create ambiguity, and what missing details will delay billing.
The third failure is waiting for denials to reveal workflow gaps. Denials are lagging indicators. By the time they appear, staff time has already been wasted, accounts receivable has already been delayed, and management confidence is already damaged. Smart teams use pre-bill edits, focused audits, and early trend reviews tied to EOB interpretation, coordination of benefits, patient responsibility terms, and Medicare reimbursement understanding.
The fourth failure is separating compliance and operations. A release is often pushed into a compliance folder while billing managers focus on production and collectors focus on follow-up. That split is dangerous. A coding change is a compliance matter because accuracy matters. It is also an operations matter because delay, denial, and rework matter. Teams that integrate both lenses outperform teams that isolate them. That is why it helps to connect change management to surgical coding compliance terms, billing compliance violations and penalties, compliance audit trends, and coding error trends.
The fifth failure is failing to measure adoption. Leaders often ask whether the update training happened. The better question is whether behavior changed. Did coders shift to the new code set correctly? Did denial rates improve or worsen? Did providers supply the missing specificity? Did edit overrides drop? Did rework volume rise? Without that measurement, implementation becomes a checkbox exercise instead of a performance discipline.
5. Best Practices for Coders, Auditors, and Revenue Teams When New Releases Go Live
When an update goes live, the goal is not merely “use the new codes.” The goal is to stabilize accuracy fast while protecting productivity and reimbursement. That requires a practical go-live playbook.
Start with a high-risk list. Identify the top twenty to fifty code families, service lines, or claim scenarios most likely to be affected. Those should receive focused pre-go-live review and post-go-live monitoring. For many teams, that means high-volume office visits, chronic disease diagnoses, imaging, injections, specialty procedures, telehealth encounters, and services with known payer sensitivity. This approach works better than generic all-staff education because it concentrates attention where financial exposure is real.
Next, establish a two-week rapid feedback loop. Coders need a fast way to escalate ambiguous charts, confusing payer outcomes, and documentation gaps. Supervisors need a way to push clarifications back to the team without waiting for the next monthly meeting. Educators need to convert repeat errors into short refreshers. Auditors need to sample the new patterns early. This kind of loop strengthens both coding education and training terms and career development for coders because it trains professionals in live analytical thinking rather than passive reading.
Use micro-audits instead of broad retrospective audits immediately after release. Pull a narrow sample of affected services and review them deeply. Look for old-code persistence, unsupported specificity, incorrect modifier use, payer mismatch, template gaps, and charge-capture errors. This will surface implementation failure much sooner than a general quarterly audit. Pair those reviews with SOAP note and coding guidance, query process terms, CDI terminology, and coding certification terms.
Build a release library that coders can actually use. Not a cluttered shared drive full of PDFs no one opens, but a structured reference containing: what changed, effective date, affected specialties, affected payers if applicable, chart examples, documentation tips, denial watch items, and system build status. Over time, this becomes one of the most valuable assets in the department because it reduces relearning and supports onboarding. It also aligns well with online resources and communities for exam prep, continuing education units for coders, coding credentialing organizations, and expert certification strategies.
Finally, think beyond annual survival. Teams that master coding releases become stronger in every adjacent area: payer analysis, edit management, denial prevention, clinical communication, audit readiness, and leadership credibility. That is part of why professionals who understand update implementation deeply often grow into broader roles in revenue cycle management, director of coding operations pathways, and even the future of medical coding with AI. Systems change will keep accelerating. The professionals who can absorb and operationalize change will keep gaining value.
6. FAQs About Medical Coding System Updates & Releases
-
Different parts of the coding environment update on different timelines. Major diagnosis and procedure code sets often have annual release cycles, while some HCPCS and drug-related changes can occur more frequently, and payer policies, edit logic, and clearinghouse requirements may shift throughout the year. That is why coders should monitor not only code books, but also clearinghouse terminology, claims management, medical coding automation terms, and regulatory compliance changes.
-
The biggest risk is not just one denied claim. It is systematic error across many claims before anyone notices. A missed update can trigger repeat denials, rework, underpayments, unsupported reporting, productivity loss, and audit exposure at the same time. That risk becomes larger when teams do not connect updates to revenue leakage prevention, CARCs, RARCs, and revenue cycle KPIs.
-
Encoder software is useful, but it should never be treated as the only control. Vendors may implement updates differently, local configurations may lag, and operational workflows may still point staff toward outdated choices. Coders should validate vendor tools against official guidance and department policy while keeping a strong grasp of encoder software terms, EHR integration terms, billing system terms, and workflow terms.
-
Keep it short, chart-focused, and consequence-based. Providers respond best when they understand exactly what changed, what documentation detail is now required, what phrases create ambiguity, and how missing details delay billing or create queries. A one-page specialty summary tied to CDI terms, SOAP note guidance, query process standards, and medical necessity criteria usually works better than a long presentation.
-
Audit the highest-volume and highest-risk services first. Look for deleted code use, unsupported specificity, old modifier habits, payer-specific rejections, medical necessity mismatches, and charge build failures. The first audit sample should be narrow and fast, not broad and delayed. That approach works especially well when paired with medical coding audit terms, claims reconciliation terms, payment posting guidance, and billing reconciliation terms.
-
Coders who can interpret releases, teach others, identify workflow risk, and protect reimbursement become far more valuable than coders who only assign codes. They develop judgment that supports auditing, education, compliance, analytics, and leadership. That is one reason update literacy can strengthen pathways into career development in coding, medical coding instructor roles, health information manager transitions, and future-proof coding careers in automation-heavy environments.