Directory of Electronic Claims Submission Platforms
Electronic claims submission platforms decide how fast a clean encounter becomes payable cash. A weak setup can hide charge capture gaps, route claims to the wrong payer, break eligibility logic, miss attachments, delay ERAs, and leave billers chasing problems that should have been stopped before transmission. This guide gives AMBCI readers a practical directory of platform types, selection criteria, workflow controls, and denial-prevention checkpoints tied to real revenue cycle management, claims management, EDI billing, and clearinghouse terminology.
1. Why Electronic Claims Submission Platforms Matter in Medical Billing
Electronic claims submission platforms sit between the provider’s documentation, coding, charge entry, payer rules, and payment posting process. When the platform is configured correctly, it catches avoidable problems before they become denials: missing member IDs, invalid diagnosis pointers, mismatched NPI/TIN data, incorrect place of service, bad modifier sequencing, stale payer IDs, incomplete prior authorization fields, and inconsistent claim form mapping. That is why strong billers connect platform selection to accurate medical billing and reimbursement, coding edits and modifiers, medical necessity criteria, and charge capture controls.
The biggest mistake practices make is treating claims submission as a “send button.” Submission quality begins before the claim leaves the billing system. The platform must know which form type applies, whether the claim belongs on a professional or institutional route, which payer companion guide requirements matter, which edits must fire before submission, and how rejected claims return to the team. A billing department that understands CMS-1500 form terms, UB-04 billing form requirements, healthcare billing acronyms, and medical coding workflow terms can separate platform issues from documentation issues, payer issues, and staff training issues.
A high-performing submission platform should reduce avoidable rework. It should show claim status clearly, separate front-end rejections from payer denials, give useful rejection reasons, support batch management, track aging, and connect remittance data back to the original encounter. Without that visibility, teams waste hours opening payer portals, reading vague rejection notices, and guessing whether the problem belongs to eligibility, coding, credentialing, payer enrollment, or payment posting. The best approach links submission technology with advanced claims reconciliation, payment posting, EOB interpretation, and CARC code analysis.
Electronic Claims Submission Platforms Directory: What Each Type Does and Where It Fits
| Platform Type | What It Handles | Billing Risk It Controls | Best Practice Action |
|---|---|---|---|
| Clearinghouse portal | Routes electronic claims to multiple payers using payer IDs and EDI rules | Bad routing, missing payer enrollment, front-end rejections | Map every payer using clearinghouse terminology and verify payer ID changes monthly |
| Practice management claims module | Builds, edits, batches, submits, and tracks claims from billing records | Charge lag, missing claim data, weak batch visibility | Tie workflows to practice management systems and daily claim release queues |
| EHR-integrated submission tool | Transfers chart, diagnosis, procedure, provider, and encounter data into billing | Documentation gaps, wrong diagnosis linking, incomplete encounter data | Audit handoffs with EHR integration terms and claim validation reports |
| RCM software platform | Combines claims, denials, payments, aging, reporting, and staff queues | Fragmented follow-up, hidden revenue leakage, poor accountability | Use RCM software terms to define ownership for every queue |
| Payer portal submission | Lets billers submit claims directly through payer websites | Manual entry errors, inconsistent tracking, missed screenshots | Reserve portals for exceptions and reconcile through billing reconciliation |
| Medicare claims submission route | Supports Medicare-specific payer rules, edits, and enrollment requirements | Medicare rejections, documentation mismatch, reimbursement delays | Validate against Medicare reimbursement and Medicare documentation requirements |
| Medicaid claims submission route | Handles state-specific eligibility, program, and managed care requirements | Wrong payer path, plan mismatch, missing authorization data | Build payer-specific checklists inside healthcare claims management workflows |
| Commercial insurance submission platform | Routes claims to private payers, networks, and employer-sponsored plans | COB errors, plan mismatch, contract underpayment | Pair submission rules with commercial insurance billing terms |
| Dental-medical crossover platform | Supports claims that require medical billing logic for oral or maxillofacial services | Wrong benefit path, rejected procedure mapping, weak medical necessity support | Check diagnosis support through medical necessity criteria |
| Institutional claims tool | Creates UB-04/837I claims for facilities, hospitals, and institutional settings | Revenue code errors, type of bill errors, occurrence code problems | Use UB-04 billing form guidance for field-level review |
| Professional claims tool | Creates CMS-1500/837P claims for physician and outpatient professional billing | Rendering provider errors, modifier errors, diagnosis pointer errors | Audit against CMS-1500 form terms |
| Eligibility-connected claims tool | Checks coverage before claim release and flags inactive or mismatched plans | Patient responsibility errors, wrong payer billing, avoidable denials | Connect eligibility findings to patient responsibility terms |
| Claim scrubber | Applies coding, demographic, payer, NCCI-style, modifier, and field-level edits | Preventable denials, compliance exposure, repeated rejections | Align edits with coding edits and modifiers |
| Attachment submission platform | Sends records, operative notes, medical necessity documents, and payer-requested attachments | Claim pends, medical review delays, missing documentation denials | Standardize proof using medical record retention rules |
| ERA/EFT-enabled claims platform | Receives electronic remittance and supports electronic payment workflows | Manual posting errors, missed underpayments, slow cash reconciliation | Train staff on RARCs and CARCs |
| Denial management platform | Categorizes denials, assigns appeals, and tracks root causes | Repeat denials, missed appeal deadlines, weak payer feedback loops | Connect denial trends to revenue leakage prevention |
| Payment posting-integrated platform | Links remits, contractual adjustments, patient balance, and claim status | Incorrect balances, bad write-offs, unresolved credits | Use payment posting controls after every ERA import |
| Analytics and reporting layer | Tracks rejection rates, denial rates, clean claim rate, days in AR, and payer trends | Invisible operational failure, weak manager oversight, late intervention | Build dashboards using RCM metrics and KPIs |
| Small practice claims platform | Combines basic claim creation, eligibility, submission, and ERA review for lean teams | Staff overload, missed rejections, inconsistent follow-up | Create daily routines around RCM terms |
| Specialty billing platform | Supports specialty edits for cardiology, radiology, lab, anesthesia, infusion, ambulance, and similar areas | Specialty-specific denials and documentation mismatch | Match platform edits to specialty references like cardiology CPT coding and radiology CPT coding |
| Telemedicine claims platform | Handles telehealth place of service, modifier, payer, and documentation requirements | Telehealth modifier denials, coverage mismatch, policy confusion | Configure rules from telemedicine coding terms |
| Behavioral health claims platform | Supports therapy, psychiatric, session-based, and authorization-sensitive billing | Duration mismatch, authorization gaps, diagnosis-policy conflicts | Pair claim rules with behavioral health billing terms |
| Lab and pathology claims platform | Handles ordering provider, diagnosis support, frequency edits, and lab-specific rules | Medical necessity denials, missing ordering data, frequency denials | Use lab and pathology coding essentials |
| Ambulance claims platform | Supports origin/destination, mileage, medical necessity, and transport documentation | Trip documentation denials, modifier problems, mileage issues | Build checks from ambulance and emergency transport coding |
| Compliance-focused claims platform | Adds audit trails, access controls, edit history, and compliance reporting | Weak evidence, privacy risk, audit vulnerability | Align controls with coding regulatory compliance |
| Security-centered submission platform | Protects claim data, user access, PHI movement, and system activity logs | Unauthorized access, PHI exposure, weak vendor governance | Review platform controls through healthcare data security terms |
| Automation-enabled claims platform | Uses rules, queues, exception logic, and automated claim status updates | Over-automation, unreviewed errors, staff blind spots | Control automation through medical coding automation terms |
| Training and education platform layer | Supports staff learning, workflow documentation, rejection interpretation, and competency checks | Knowledge gaps, inconsistent handling, repeated avoidable errors | Link workflows to coding competency assessment |
2. How to Choose the Right Electronic Claims Submission Platform
Start with claim volume, payer mix, specialty complexity, staff capacity, and denial patterns. A small primary care office may need a clean, simple platform with strong eligibility, payer ID lookup, batch submission, and easy ERA review. A multi-specialty group needs deeper edits, specialty rules, provider enrollment tracking, dashboard reporting, and denial work queues. A facility billing team needs institutional claim logic, revenue code validation, occurrence and condition code support, and close alignment with UB-04 billing terms, cost reporting, HIM terms, and utilization review terms.
A platform should make the problem visible before it makes the claim movable. That means clear front-end edits, payer-specific rejection descriptions, claim-level status, batch-level status, attachment prompts, and denial categorization. A biller should be able to tell whether a claim failed because the provider was inactive with the payer, the subscriber data was wrong, the modifier was incompatible, the diagnosis did not support the service, or the payer wanted documentation. Strong teams connect platform alerts to clinical documentation improvement terms, coding query process terms, SOAP notes and coding, and problem list documentation.
Integration matters more than the sales demo usually suggests. If the EHR sends bad provider data, old insurance, missing diagnosis pointers, or incomplete encounter fields, the claims platform becomes a prettier place to find the same failure. The evaluation should include test claims from real workflows: new patients, secondary claims, corrected claims, high-dollar procedures, authorization-heavy visits, telemedicine encounters, bundled services, preventive visits, and specialty claims. Testing should include coordination of benefits, patient responsibility, preventive medicine CPT coding, and CPT modifier usage.
Reporting is the deciding factor for serious revenue cycle teams. A platform should show rejection rate by payer, denial rate by category, average days from encounter to submission, claims held by edit type, claims pending attachment, ERA posting status, unresolved rejections, and staff productivity. Without those metrics, managers rely on anecdotes from the loudest payer problem of the week. With metrics, they can fix the root issue: missing registration fields, weak coding education, poor provider documentation, payer enrollment gaps, or bad clearinghouse setup. That is where RCM metrics and KPIs, data analytics and reporting, claims reconciliation, and revenue leakage prevention become daily operating tools.
3. The Claim Submission Workflow a Strong Platform Should Support
A clean electronic claim begins with accurate patient registration. The platform should receive the correct legal name, date of birth, subscriber number, group number, payer, plan type, relationship to subscriber, accident indicators, and secondary coverage details. One wrong field can turn a payable claim into a rejected transaction that sits untouched for days. The strongest offices train front-desk and billing teams together so eligibility, COB rules, patient responsibility terms, and commercial insurance billing stay connected from intake to claim release.
The next control point is documentation. A claim may pass technical edits and still fail payer review when the chart does not support the billed service. The platform should help the team identify documentation-sensitive claims before submission: high-dollar procedures, time-based services, medical necessity-sensitive labs, ambulance transports, infusion services, and procedures needing laterality, anatomical detail, or diagnosis specificity. That requires billers to understand medical necessity criteria, CDI terminology, medical record retention, and surgical coding compliance.
Charge entry comes next. The platform should detect inconsistent units, duplicated charges, missing modifiers, mismatched diagnosis pointers, payer-specific procedure rules, and incompatible place-of-service logic. It should also allow supervisors to review held claims without forcing every correction into a slow manual process. Specialty workflows need deeper controls: cardiology CPT coding, emergency medicine CPT codes, gastroenterology coding, and radiology billing and coding terms should influence edit configuration.
After submission, the platform must separate rejections, acknowledgments, payer accepts, pends, denials, and remittance outcomes. This distinction protects staff time. A clearinghouse rejection often means the claim never reached the payer. A payer denial means the payer adjudicated and refused payment. An ERA adjustment may represent contractual reduction, patient responsibility, bundling, medical necessity, timely filing, or missing information. The platform should connect every outcome to EOB guidance, RARCs, CARCs, and payment posting controls.
Quick Poll: What is your biggest electronic claims submission pain right now?
4. Platform Features That Prevent Rejections, Denials, and Revenue Leakage
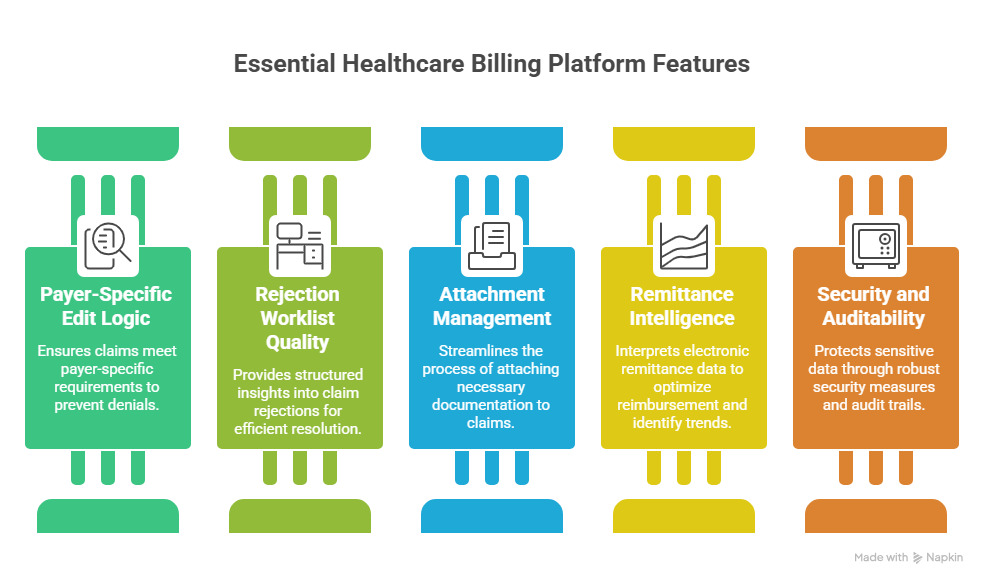
The first feature to demand is payer-specific edit logic. Generic edits catch obvious missing fields. Strong payer edits catch the painful details: payer-specific modifiers, authorization requirements, diagnosis policies, timely filing rules, claim frequency rules, provider taxonomy requirements, and attachment triggers. If the platform lets every questionable claim leave the door, billers inherit a denial queue that should have been prevented. This is why platform configuration must reflect coding regulatory compliance, medical coding audit terms, coding ethics and standards, and modifier usage examples.
The second feature is rejection worklist quality. A rejected claim should not fall into a general bucket with vague language. The platform should show rejection source, rejection code, responsible team, correction field, date received, resubmission history, and escalation path. It should also distinguish demographic fixes from coding fixes, payer setup fixes, provider enrollment fixes, and documentation fixes. That structure turns chaos into workflow. It also protects the team from correcting the same symptom repeatedly while the root cause remains untouched. Connect these queues to medical coding workflow terms, healthcare claims management, billing reconciliation terms, and revenue cycle KPIs.
The third feature is attachment and documentation management. High-risk claims often need operative reports, itemized statements, lab results, referrals, authorizations, medical necessity documentation, therapy notes, or transport records. A platform that flags attachment needs before submission can prevent pends and reduce payer back-and-forth. This matters heavily in infusion and injection therapy billing, dialysis coding terms, ambulance coding, and hospice and palliative care coding.
The fourth feature is remittance intelligence. Electronic submission loses value when the team cannot interpret what came back. A strong platform should connect ERA data to posted payments, adjustments, secondary claims, patient balances, refunds, underpayments, and denial appeals. It should help staff compare expected reimbursement to actual reimbursement and identify repeated payer behavior. This protects cash by turning remittance data into action. The platform should support workflows built around EOB interpretation, claim adjustment reason codes, remittance advice remark codes, and advanced claims reconciliation.
The fifth feature is security and auditability. Claims contain protected health information, financial data, provider identifiers, and payer details. The platform should support role-based access, user activity logs, secure transmission, vendor accountability, access reviews, and data retention practices. A team should know who edited a claim, who released it, what changed, when it was submitted, when it was accepted, and what proof supports the action. This protects both reimbursement and compliance. Build these standards around healthcare data security terms, electronic medical record documentation terms, HIM terms, and coding compliance guidance.
5. Common Platform Mistakes Billing Teams Should Fix First
One common mistake is allowing claims to be released without ownership rules. Every hold should have an owner: registration, coding, provider documentation, billing, credentialing, authorization, or payment posting. Without ownership, claims sit in “pending” status while everyone assumes someone else is handling them. A proper platform setup should define who clears demographic edits, who corrects coding edits, who contacts providers for documentation, who manages payer enrollment, and who follows rejected claims. This turns practice management system terms, RCM software terms, coding education terms, and coding competency assessment into measurable operations.
Another mistake is treating clearinghouse acceptance as payment progress. Acceptance only confirms the claim passed a front-end step. It does not prove medical necessity, contract accuracy, authorization validity, patient eligibility, or final reimbursement. Teams that stop monitoring after acceptance often discover problems when AR has already aged. A strong workflow continues from submission to payer acknowledgment, claim status, remittance, payment posting, secondary billing, patient balance transfer, and reconciliation. This full path requires comfort with EDI billing terms, clearinghouse terminology, payment posting, and collections and bad debt.
A third mistake is ignoring specialty configuration. A generic claim scrubber may miss radiology supervision requirements, anesthesia time logic, ambulance origin/destination documentation, infusion drug units, lab diagnosis frequency edits, or behavioral health session rules. The platform should support the specialty’s highest-risk billing points. A multi-specialty group should maintain specialty-specific edit review, documentation checklists, and denial dashboards. Use specialty references such as anesthesia billing terms, lab and pathology coding, sleep medicine billing, and speech-language pathology coding.
The final mistake is measuring staff productivity without measuring claim quality. A team can submit many claims and still create cash delays if rejection rates, denial rates, and resubmission rates are high. Better metrics include clean claim rate, first-pass acceptance rate, rejection resolution time, denial overturn rate, claim lag, days in AR, underpayment recovery, and payer-specific preventable denial trends. This is where leaders need data analytics and reporting terms, RCM metrics and KPIs, revenue leakage prevention, and billing reconciliation.
6. FAQs About Electronic Claims Submission Platforms
-
An electronic claims submission platform moves claims from the provider’s billing system to payers while applying routing, formatting, editing, tracking, and reporting controls. Its purpose is to help the billing team send cleaner claims, catch preventable errors earlier, and follow each claim through acceptance, denial, remittance, and payment posting. The best platforms support EDI billing, healthcare claims management, payment posting, and claims reconciliation.
-
A clearinghouse is one type of claims submission platform, but many billing systems also include claims modules, scrubbers, payer portals, ERA tools, denial worklists, and reporting dashboards. A clearinghouse mainly routes electronic claims and returns acknowledgments or rejections. A broader platform may also manage eligibility, claim edits, attachments, ERAs, denial queues, and analytics. Billers should understand clearinghouse terminology, RCM software terms, practice management systems, and EHR integration terms.
-
The team should check payer connectivity, eligibility integration, claim scrubbing, payer-specific edits, provider enrollment support, attachment handling, ERA/EFT workflow, denial management, reporting, security, audit trails, and support quality. The platform should also fit the specialty, payer mix, volume, and staffing model. A serious evaluation uses live workflow tests tied to CMS-1500 terms, UB-04 terms, coding edits, and medical necessity.
-
Submission edits usually catch formatting, missing data, routing, and some coding problems. Payer denials may still happen because coverage ended, authorization was missing, documentation did not support the service, medical necessity was weak, benefits were coordinated incorrectly, or the payer applied contract and policy rules after adjudication. That is why billing teams must connect submission tools with EOB review, CARC analysis, RARC interpretation, and regulatory compliance.
-
A platform reduces revenue leakage when it catches missing charges, prevents avoidable rejections, flags underpayments, tracks unresolved denials, supports timely resubmission, and shows managers where cash is getting stuck. The platform must create visibility across claim creation, submission, rejection correction, payer adjudication, remittance review, payment posting, and reconciliation. Strong teams pair the technology with charge capture terms, revenue leakage prevention, RCM KPIs, and billing reconciliation terms.
-
AMBCI learners should focus on claim form structure, payer routing, EDI basics, clearinghouse rejections, claim edits, denial codes, remittance interpretation, payment posting, reconciliation, and compliance documentation. They should practice reading claim errors the way working billers do: identify the source, find the failed field, correct the root cause, resubmit cleanly, and document the resolution. That skill connects directly to medical coding workflow, coding career development, CBCS exam terms, and coding credentialing organizations.